Claim Denials Are Draining Your Revenue
Recover your share. Reduce denials by 15-40%, accelerate cash flow, and recover millions annually—without adding staff.
A ready-built, fully customizable HealthFAX module that replaces months of custom development with an AI engine purpose-built for revenue cycle optimization.
Improve First-Pass Acceptance Rates
Our advanced AI analyzes millions of claims to identify optimization opportunities and improve submission accuracy in real-time. Healthcare organizations achieve 15-40% improvement in acceptance rates.
40%
Average denial reduction within first 6 months
35%
Faster cash flow cycle on average
24/7
Continuous AI monitoring and threat detection
From Revenue Leakage to Revenue Recovery
The Problem
Hundreds of billions lost annually to claim denials industry-wide
Average denial rates of 5-10% drain revenue, exhaust staff, and delay cash flow. Most organizations don't know where the leakage starts.
The Old Way
Manual reviews, reactive denial management, custom builds
Months of custom development, fragmented tools, and armies of coders chasing denials after they happen. Expensive, slow, and error-prone.
The HealthFAX Way
Ready-built AI that predicts and prevents denials
Deploy in weeks. AI analyzes claims before submission, flags risks in real-time, and adapts to your payer mix—fully customizable to your revenue cycle.
The Outcome
15-40% denial reduction and millions recovered annually
35% faster cash flow, continuous AI monitoring, and measurable ROI—without adding staff or building from scratch.
Why Revenue Intelligence Matters
Maximize Reimbursement
Identify coding gaps, ensure compliance, and capture every dollar you're entitled to with intelligent claim optimization.
Drive Growth
Spot trends, forecast revenue, and make data-driven decisions that accelerate financial performance.
Prevent Denials with AI
Machine learning predicts denial risks before claims are submitted, enabling proactive corrections and recovery strategies.
Real-time Monitoring
Track revenue metrics in real-time and stay ahead of financial challenges with actionable alerts.
Powered by AI-Driven Insights
Denial Prevention Engine
Advanced AI analyzes claim characteristics, payer rules, and your organization's history to predict denials with 94% accuracy before submission.
Clinical Context Integration
Combine revenue insights with clinical data for holistic understanding of patient outcomes and financial impact.
Intelligent Recommendations
Receive specific, prioritized recommendations to improve revenue capture, reduce denials, and optimize operations.
See It In Action
Discover how HealthFAX AI Revenue Intelligence revolutionizes RCM processes
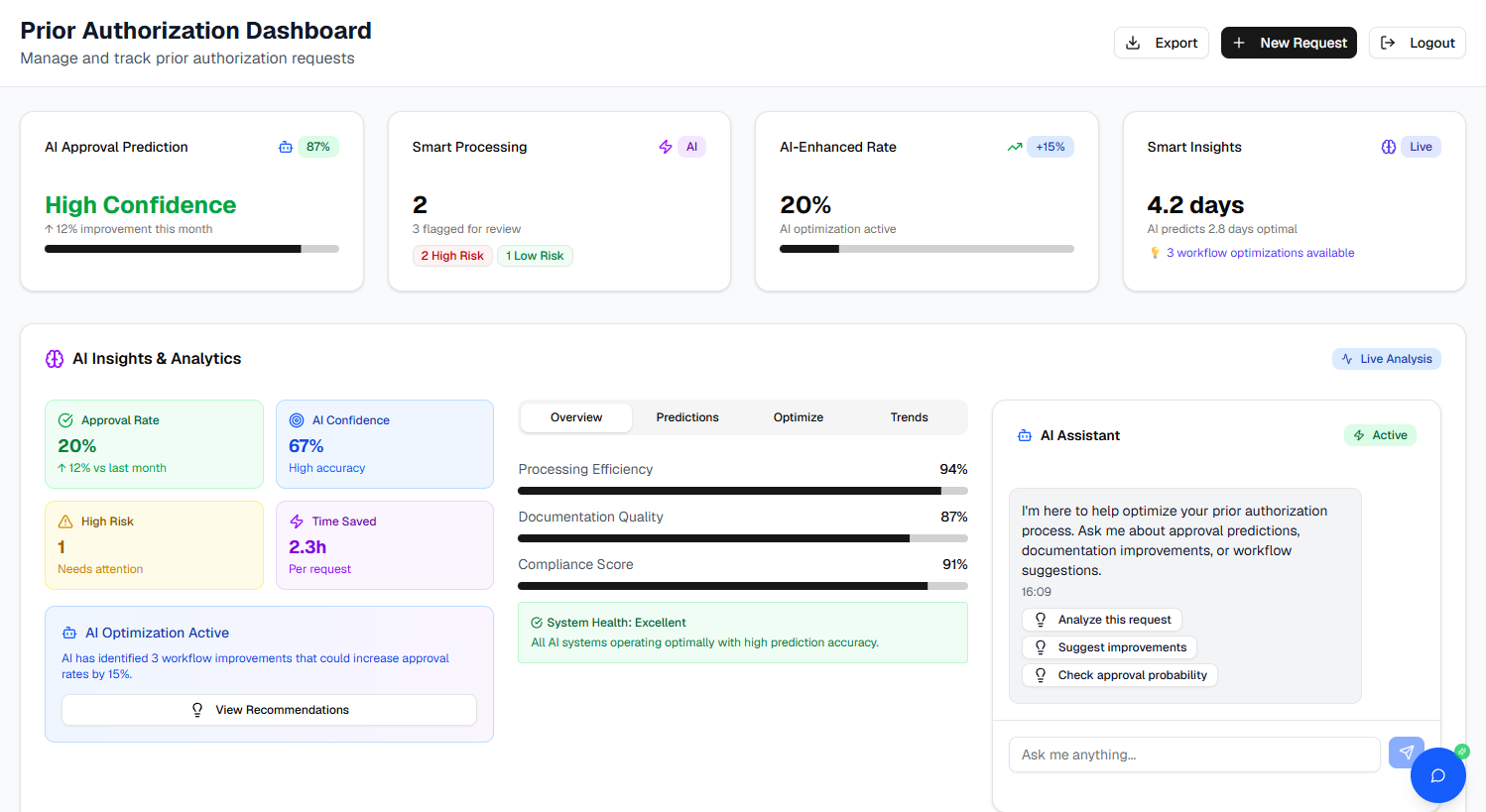
Automated Prior Auth
HealthFAX AI transforms prior authorization by automating the entire verification process in real-time. Our intelligent system instantly processes authorizations, reduces approval times from days to hours, and eliminates manual bottlenecks that delay claims. By leveraging AI to verify medical necessity and match payer requirements, you accelerate cash flow while ensuring compliance at every step of the RCM cycle.
4.2 hrs
Average approval time
100%
Auto-submitted
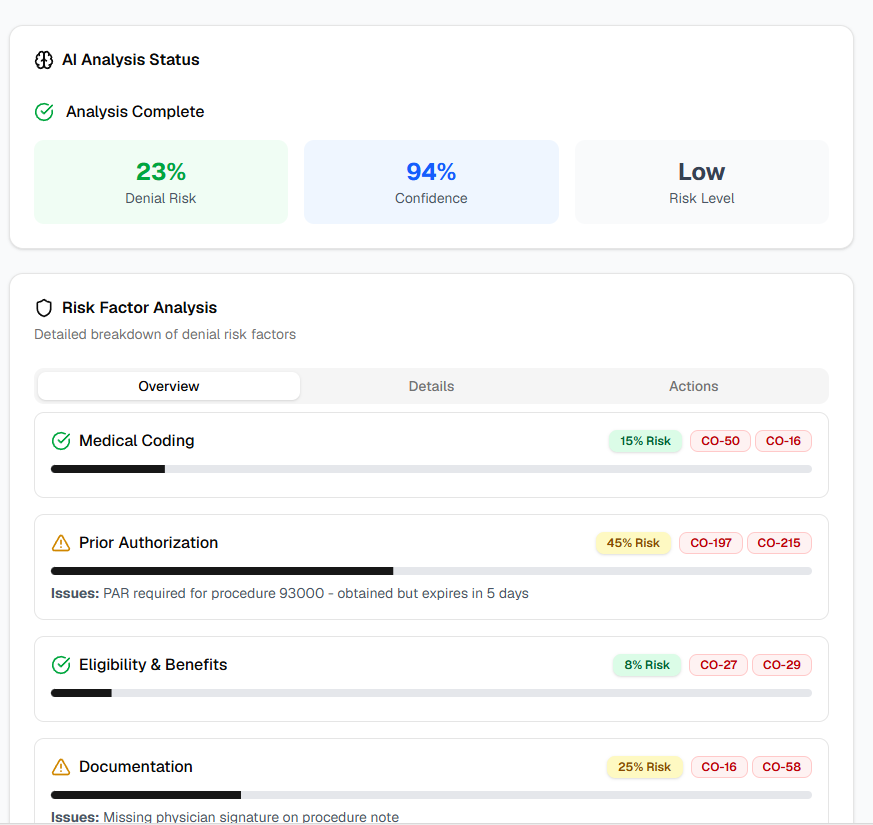
Denial Prediction
Stop denials before they devastate your revenue. HealthFAX AI Revenue Intelligence uses predictive machine learning to identify high-risk claims with exceptional accuracy, enabling proactive interventions before submission. Our system analyzes claim characteristics against payer rules and your organization's historical patterns, flagging problematic coding, missing documentation, or compliance issues in real-time. Transform denial management from reactive recovery to proactive prevention.
94%
Denial prediction accuracy
Real-time
Risk flagging before submission
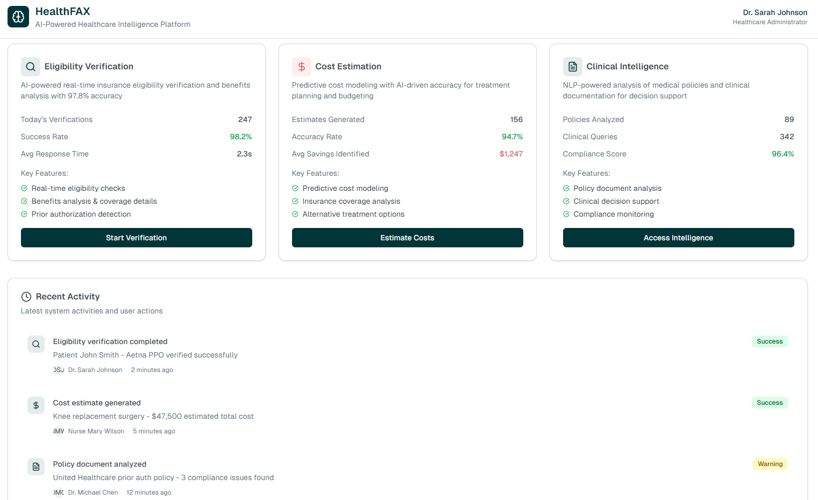
AI Cost Estimation
Maximize revenue capture with intelligent, real-time cost estimation powered by HealthFAX AI. Our system analyzes thousands of CPT codes, insurance plans, and regional pricing rules to deliver accurate reimbursement predictions before claims are submitted. By revealing expected reimbursement upfront, your team can identify high-value opportunities, make informed billing decisions, and optimize patient financial responsibility collection with confidence intervals that reflect estimation accuracy.
High
Reimbursement estimation accuracy
95.2%
Confidence level
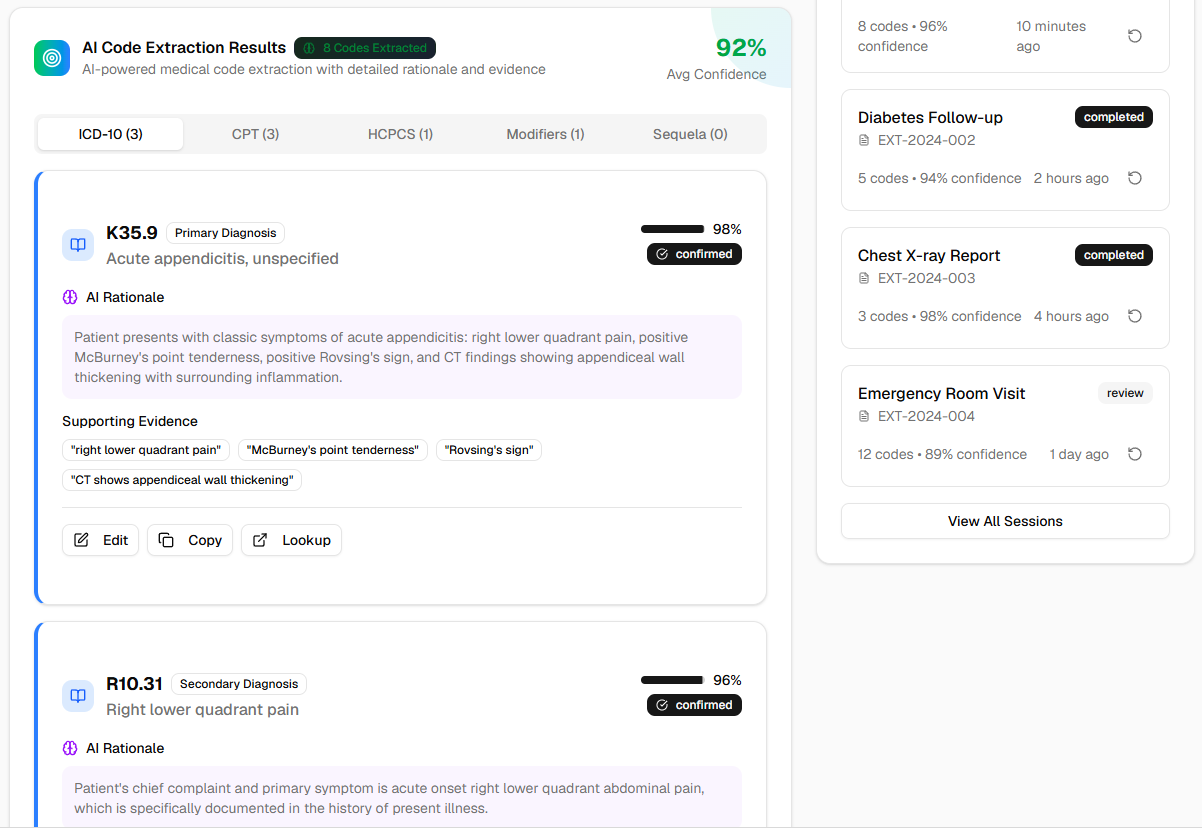
Intelligent ICD/CPT Code Assignment
Revolutionize your coding accuracy and efficiency with HealthFAX AI's intelligent code assignment system. By analyzing clinical notes with advanced natural language processing, our AI suggests the most appropriate ICD-10 and CPT codes while catching common coding errors before claim submission. This eliminates compliance risks, reduces manual coding workload, and ensures every code reflects the full clinical picture—maximizing legitimate reimbursement while maintaining audit-ready documentation standards across your entire RCM operation.
Watch Revenue Intelligence in Action
Discover how AI-powered denial prediction, automated prior auth, intelligent cost estimation, and autonomous coding work together to maximize reimbursement and transform your revenue cycle.
Platform Overview
Watch how our AI-powered platform delivers intelligent insights across clinical and revenue domains, enabling coordinated action that transforms healthcare operations.
Ready to Transform Your Revenue Strategy?
Join leading healthcare organizations leveraging AI-powered insights to optimize reimbursement and drive growth.